Inverse Incentives: Why PBMs Profit When Your Spending Soars
Written by
SmithRx
Key Takeaways
Legacy PBMs use practices like spread pricing to increase their profits as your pharmacy costs rise.
Vertical integration lets PBMs steer members toward their own high-cost pharmacies to pad their bottom line.
Modern, transparent models align interests by focusing on the lowest net drug cost for your plan.
Unless you’re incredibly involved in the benefits selection process for your organization, or a benefits professional yourself, you may, justifiably, assume that the vendors you choose are negotiating the best prices for your plan and members. After all, that’s what pharmacy benefits managers (PBMs) were designed to do. Yet, the industry has morphed and created a system where employers and patients are left paying more than ever before, while being told they’re getting fantastic deals and discounts.
How is that possible? Through mergers, acquisitions, and a complex web of vertical integration, a few behemoth companies now own every vertical in the healthcare industry (insurance, pharmacy benefits, pharmacies, and even private-label manufacturing). To suit their own interests exclusively, they’ve created a system of inverse incentives: when plans pay more they earn more. This compensation structure makes it disadvantageous for PBMs to prioritize lowest-net cost drugs, and as a result, plans literally pay the price.
Let’s explore how legacy PBMs warped incentives manifest in practices, why vertical is harmful (and not “easier” for member navigation), and why placing trust in discount-based pricing structures is a risky financial move.
Legacy Tactics: Spread Pricing & Supply Chain Monopoly
The largest PBMs will rely on their sheer ubiquity and long-standing reputation for being “irreplaceable” to keep their clients. There’s a misconception that, for larger employers, it simply isn’t worth the headache of transitioning to a new PBM. Unlike more transparent, pass-through alternatives, they don’t want CFOs and CHROs asking to check under the hood of how they operate. The Big Three placate leaders with promises of staggering discounts or rebates that look great on paper, but bills end up blowing benefits budgets out of the water.
This bait and switch is achieved through a few particularly misleading practices to which modern PBMs, like SmithRx, are fundamentally opposed. They include:
Spread Pricing: This is the practice of charging an employer, or plan, one price for a drug claim while paying the pharmacy a lower amount. The PBM pockets the difference, or spread, as an undisclosed source of profit. You aren’t paying for the actual cost of medications; you’re paying an untraceable, unauditable markup that isn’t reflected in your invoices.
Vertical Integration: The largest PBMs are owned by the same parent companies that own the largest health insurers and pharmacies too. This creates a captive supply chain where the PBM is incentivized to steer your members toward their own ‘high-cost’ pharmacies. This self-dealing eliminates crucial market competition and almost ensures that even if a lower net cost option (either pharmacy or even drug) exists, your plan goes down PBM’s own most profitable ‘internal’ channel.
Rebate Retention: While many PBMs, even legacy ones, now tout that they are “100% rebate pass-through,” they often hide true plan economics through opaque accounting. By reclassifying rebates as other fees, PBMs can then keep a massive portion of the savings for themselves. More dangerously, it incentivizes the benefit manager to favor high-cost brand drugs because they often come with large rebates. Looking closely at the math, it’s often that a generic exists that would cost your plan less than a “preferred” brand medication even with a large rebate.
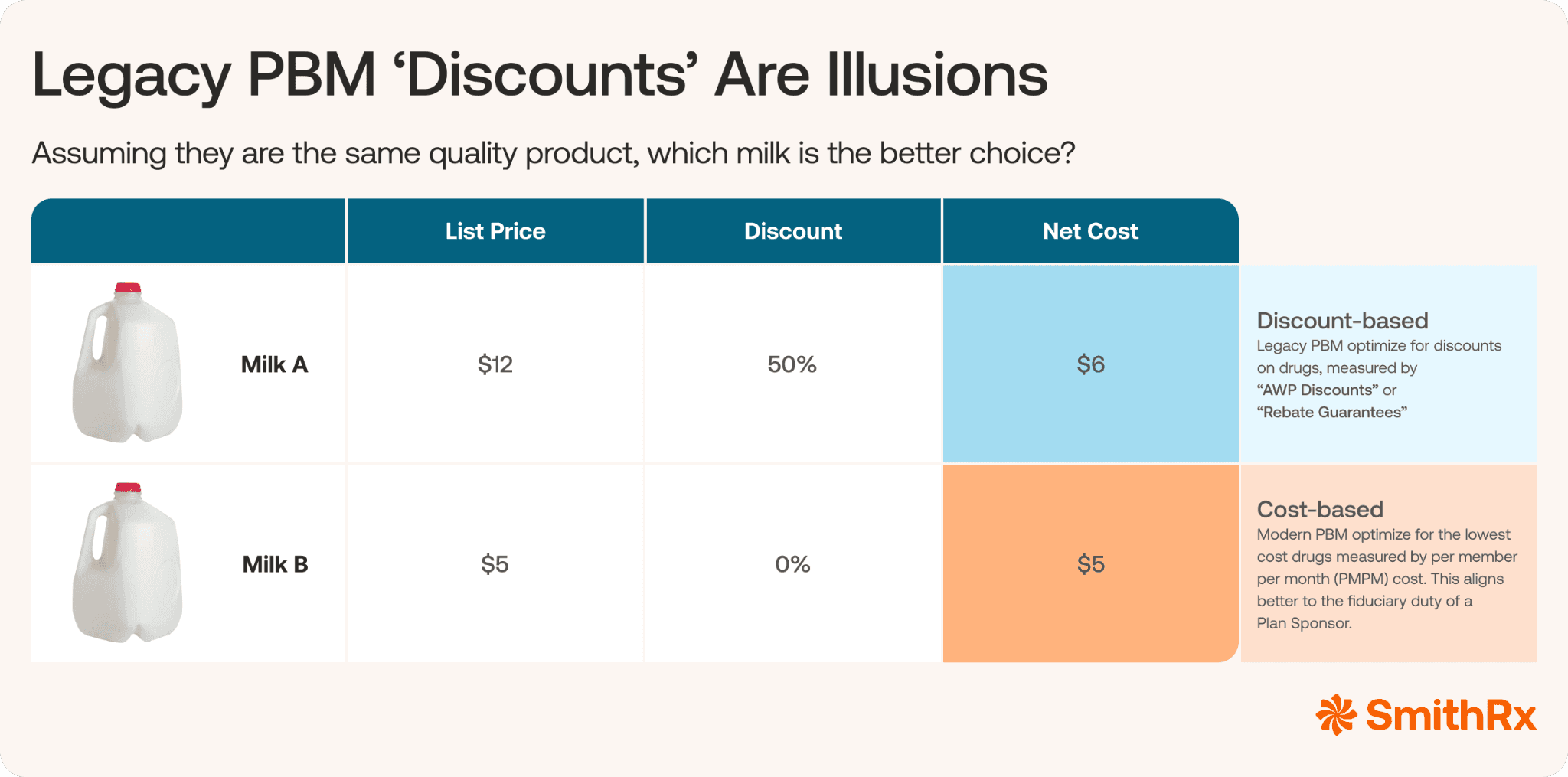
Modern Mission: Radical Transparency, Total Alignment, Lowest Net Costs
The modern alternative to discount-based models is the cost-based model. This model relies on fixed-fee economics that fundamentally align PBM performance with employer outcomes. Rather than making money off of higher drug prices, modern PBMs are instead paid a flat, transparent administrative fee per member, per month. This radical model delivers much needed:
Simplicity: Modern PBMs don’t make money off of hidden margins. Every dollar of discount and every cent of rebate is passed directly back to you.
Alignment: With a modern, fixed-fee model, the PBM only ‘wins’ when their clients get excellent member service and lower costs to retain business.
Consistency: In a completely transparent model, there’s no playing favorites or using certain clients’ higher costs to offset another’s subsidized rates. Every plan gets the lowest net cost, every time.
Checking Your PBM’s Math: Demand PMPM-Based Metrics
At a glance, legacy PBM proposals look great; maybe even too good to be true. Legacy, and even some so-called “pass-through” PBMs are notorious for gaining business using vanity metrics such as high rebate percentages or aggressive discounts off of Average Wholesale Prices (AWP). As illustrated above, a 50% discount on a drug that is priced 140% higher than its generic equivalent is a net loss for your company.
It is not financially advantageous to select a benefit partner who touts discounts as the end-all-be-all. For plan sustainability and cost-control, the north star has to be the lowest net cost. In practice, this means pushing your PBM to report the total spend, subtracting 100% of the rebates, and measuring the final PMPM (Per Member Per Month) cost.
If your PBM is steering members toward high-cost brand-name drugs just to ‘capture’ a larger rebate that they partially retain, your net cost is likely ballooning. Your long-term plan sustainability needs a transparent model that focuses on clinical efficacy at the lowest price point, regardless of the rebate size.
The ROI of Pharmacy Benefits Transparency
The legacy PBM model is built on black box systems that make it nearly impossible to understand plan mechanics. Contracts are unnecessarily complex, and employers are often stripped of ownership over their own pharmacy data, which makes a meaningful audit impossible.
While significant pharmacy benefit reform has recently passed (such as the 2026 Consolidated Appropriations Act and the Department of Labor’s proposed rule) there is no guarantee that legacy providers won't find new loopholes to protect their margins. Forward-thinking CFOs are getting ahead of the regulatory wave by choosing partners who are already built for a transparent future.
Choosing a modern PBM, like SmithRx, ensures your plan receives:
Radical Transparency: You gain ownership of your claims data down to the individual claim level. There are no surprise fees, reclassified rebates, or hidden markups. You see exactly what the pharmacy was paid and exactly what you are being charged, turning the pharmacy benefit into a fully auditable financial line item.
Total Alignment: By utilizing a flat, per member, per month (PMPM) fee, SmithRx’s incentives are finally mirrored with yours. Instead of chasing high-rebate brand drugs to pad their own margins, a modern PBM focuses on lowest net cost by prioritizing low-cost generics, biosimilars, and clinical programs that actually drive down your total spend.
Fundamental Flexibility: You are no longer locked into restrictive network designs that favor the PBM's bottom line. You have the power to partner with best-of-breed benefits providers, provide large pharmacy networks for your population, and pivot your strategy in real-time based on actual performance.
If pharmacy spend with your legacy PBM feels unsustainable and uncontrollable, you’re not alone. Many of the nation’s largest employers have faced the same challenges and they’ve capitalized on the exceptional opportunity that modern PBMs offer.
The financial logic is straightforward: when your PBM’s incentives are aligned with your plan’s health, you eliminate the structural friction that has historically driven up costs. Moving to a model built on transparency allows you to bring value to your benefits that was previously unattainable due to misaligned interests. Ultimately, when your pharmacy benefits’ success is measured by how much you pay, rather than what you could ‘get discounted’, your organization can achieve the sustainable, meaningful savings required to serve both your bottom line and your members’ well-being.

Written by
SmithRx
SmithRx is the #1 Modern PBM, relentlessly focused on eliminating the conflicts and complexity of legacy pharmacy benefits. Built on radical transparency and fiduciary alignment, we empower employers to take control of their pharmacy spend and experience with our 100% pass-through model.



