Client Cross-Subsidization: The Hidden Cost of “Preferred” Pricing
Written by
Alan Pannier
Pharmacy benefit managers (PBMs) were put in place to solve for an increasingly complex healthcare and pharmaceutical system, and yet, the legacy PBM players have doubled down with complexity, opacity, and fiduciary misalignment of their own creation. This skewed system has reigned supreme for decades, with businesses and patients paying the price.
As legacy misalignment and games have come to light, there’s been an industry-wide push for transparency. Some modern PBMs mean this in earnest, but many legacy and pass-through pharmacy benefit managers are using the buzzword to prop up their tried and true bad actions. There cannot be true transparency without real truth. So, some PBMs may be sharing more data and information in the name of transparency, but the truth of the matter (and the cost to your business) is still being obscured.
One of the many ways these PBMs hide the truth on costs is through Client Cross-Subsidization. This is where legacy and pass-through PBMs can artificially lower costs for priority clients (often the current shiny object they are trying to win in an RFP) by passing inflated costs on to other clients (their existing clients). As non-preferred clients switch to modern vendors, the PBMs practicing client cross-subsidization are left to either raise prices for preferred clients or shoulder the financial burden.
If transparency is the new guiding principle (or at least, marketing catchphrase) of almost every PBM, why are you still footing the bill for other clients with some PBMs?
The Mechanics of the "Managed" Contract
In legacy and most pass-through models, pricing is ‘managed to contract’ or ‘managed to guarantees’ rather than being reflective of real-time market costs. This creates a disconnect where the price a PBM bills a plan is dictated by annual guarantees rather than the actual benchmark cost.
Forked Price Lists
What’s more, these PBMs often use a “forked price list” to manage different rates for different clients simultaneously. This allows them to artificially deflate costs for some clients to meet their promised contract rates while inflating costs for others to maintain staggering margins for the PBM.
This results in:
Artificial Volatility: Costs are adjusted to hit contract guarantees rather than following market trends and savings opportunities.
No Real-Time Improvement: Improvements in supply chain costs are not passed to every client as they happen.
Without a more modern approach to pricing, such as using a platform based approach that provides the actual contracted pharmacy rates for all clients, plan sponsors face the hassle of continually negotiating and pushing their PBM never really knowing if they are getting the best deal. Instead of being “billed as contracted”, their costs are manipulated to balance the PBM’s broader portfolio.
Manipulation of the Pricing Curve
Legacy, and many pass-through, PBM’s billed pricing are flat, regardless of whether the actual market cost of drugs is falling. This creates a value gap that modern PBMs aim to eliminate.
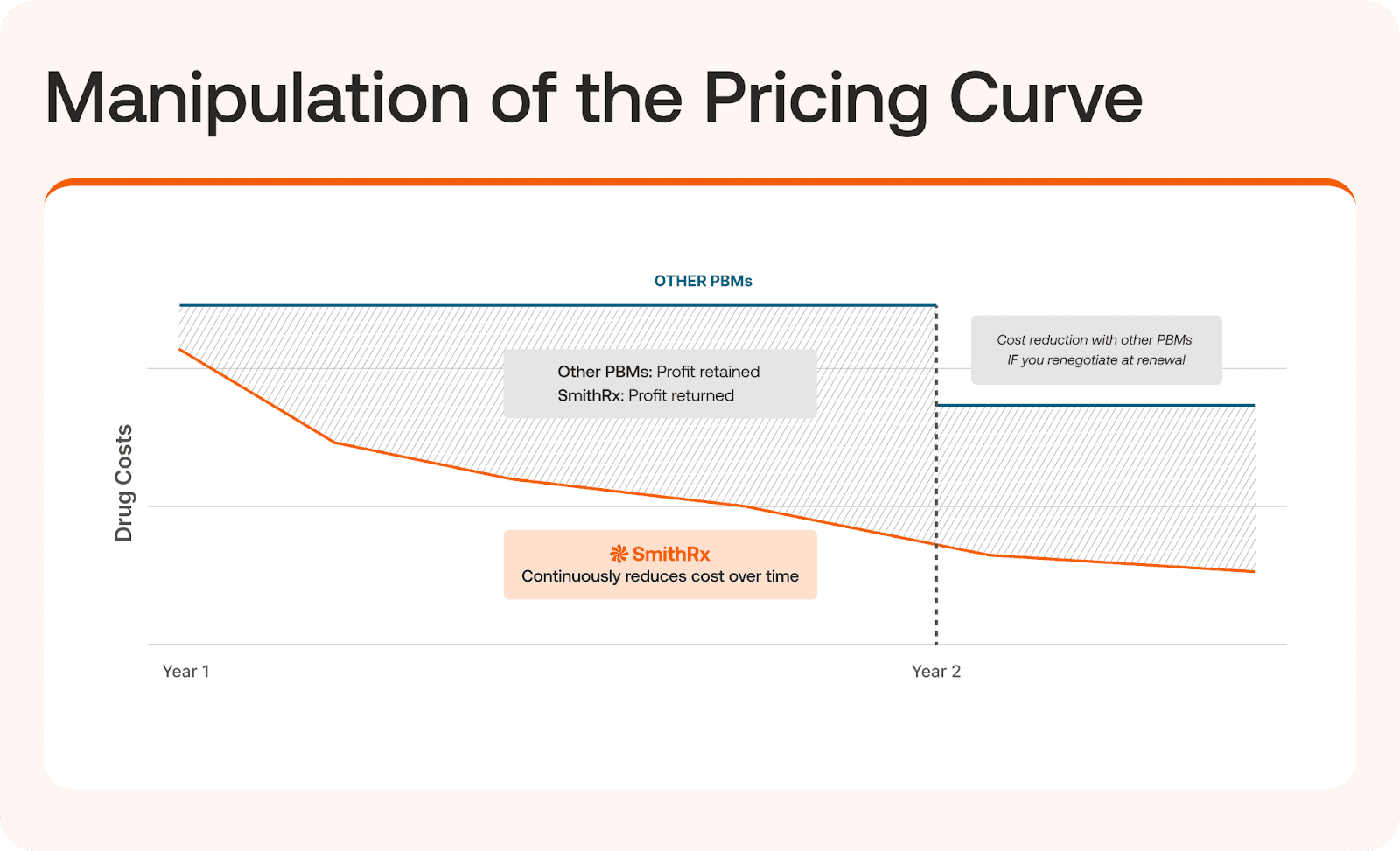
In a legacy model, a PBM sets a price at the start of a contract and keeps it static to meet specific ‘managed to contract’ guarantees. Meanwhile, the actual cost of drugs typically trends downward over time due to market efficiencies.
The difference, or space, between these two lines of average prices is “the area under the curve”. Legacy PBMs will engage in profit shifting whereby they’ll monetize this area to: keep the difference as profit and/or use it to subsidize lower prices for their established “priority” clients. Even with some pass-through models, the only way a client sees a price drop is through a renegotiation event—typically a painful, annual, or multi-year process.
In a modern model, this area isn’t monetized. Those savings are instead passed directly to the client, 100% of the time, no haggling needed.
Why the Cross-Subsidization Model is Breaking
Though almost every aspect of this system is gamed against employers, it’s still crumbling from within. What legacy players didn’t account for was the sheer number of employers opting for modern PBMs over the status quo. While the movement to modern alternatives may have started with smaller businesses making the leap of faith, today some of America’s largest employers are signing with modern PBMs.
Of course, these clients switching were the “non-preferred” clients that were paying the inflated costs. As more and more of them move away from legacy benefits managers, their subsidy pool shrinks with dire consequences.
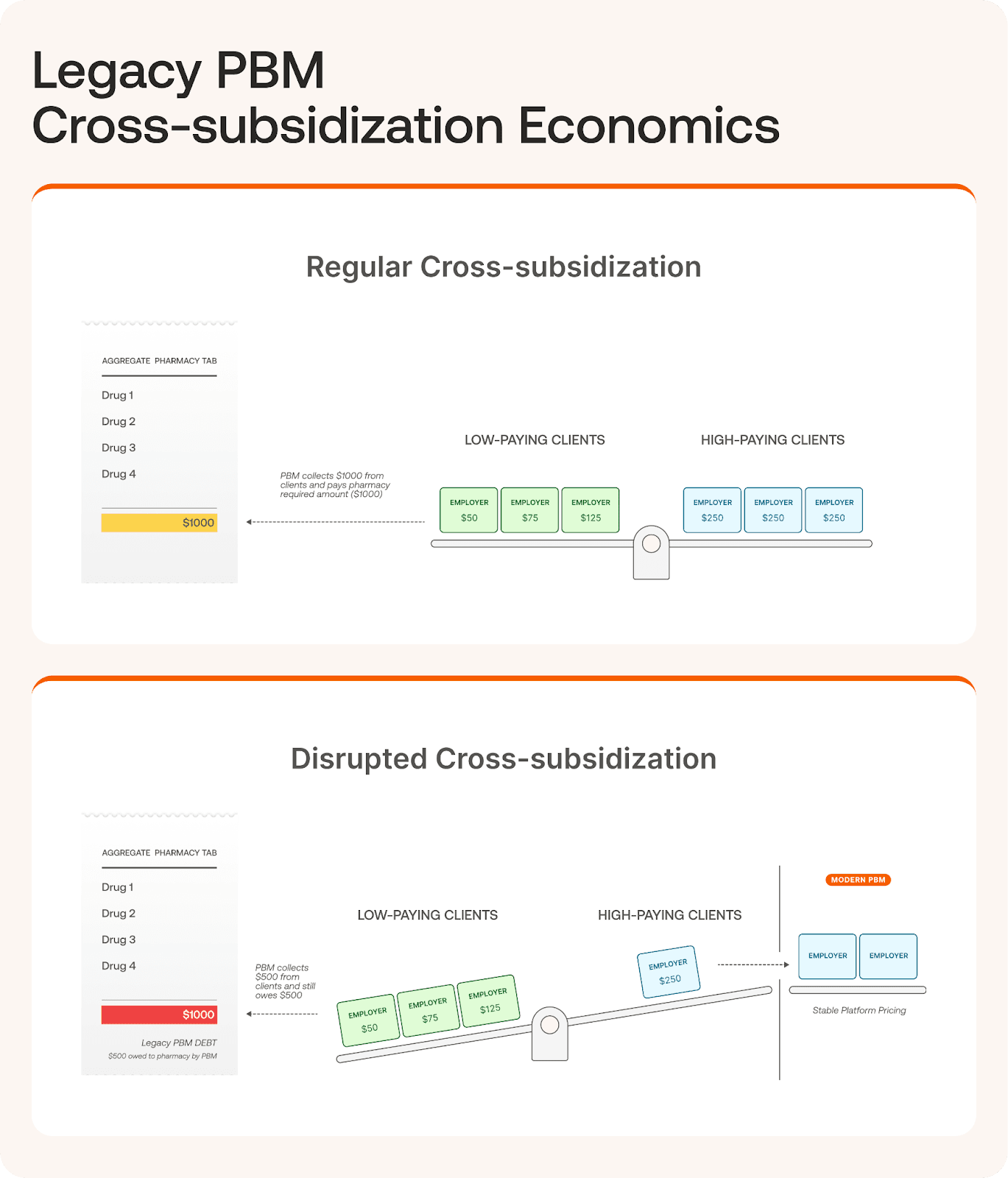
This swing in the PBM market puts the legacy managers in a corner: they can either raise prices for ‘preferred’ clients who are accustomed (and even contractually obligated to get) subsidized rates, or the PBM must shoulder the financial burden itself. Either the PBM loses a flagship client, or loses money.
A Fair Shake and Real Savings for Every Client
The future of pharmacy benefits is one free of client cross-subsidization. The more modern alternative to legacy games is a Platform Pricing model that provides direct, real-time access to the lowest net-cost drugs.
Under modern models, there’s no distinction between old and new or preferred and non-preferred clients; there’s no need to overcharge a client to play catch up with contracted rates in another client’s agreement. No one client is ‘funding’ another and instead every client is getting exceptional savings.
Modern, Platform Pricing Contract Green Flags
With so many PBMs adopting “transparency” as a marketing tactic, it can be hard to distinguish which pharmacy benefit managers will give your plan a fair shake.
Modern PBMs will have ‘green flags’ in their contract that include:
One, Single Pharmacy Price List: Every client uses the same pharmacy price list, ensuring universal supply chain transparency rather than "forked" pricing.
Billed as Contracted: Clients are billed the exact contracted rate that the PBM has with the pharmacy, eliminating supply chain profit shifting or client subsidization used to balance both pass-through and legacy PBM's books.
Continuous Improvement: While some PBMs only lower costs during a renegotiation event, modern PBMs will always be searching to take advantage of supply chain efficiencies and pass these directly to clients, rather than holding them as profit.
The “industry standard” PBM model of client cross-subsidization is a black box designed to benefit PBM margins and preferred customers at the expense of other plan sponsors. When a PBM is managing “to client contracts”, they’re prioritizing inflated guarantees over your savings and plan sustainability.
Modern platform pricing offers a better path forward: fair pricing, great savings pass-through, and more manageable pharmacy spending for plans and members alike.

Written by
Alan Pannier
Chief Strategy Officer, SmithRx
Alan oversees the company's pharmacy initiatives, including manufacturer relations, network management, and clinical solutions. His background includes clinical leadership roles at Magellan Health and Veridicus Health, as well as hands-on experience as a practicing pharmacist. Alan's academic credentials include an MBA and PharmD from Idaho State University, a Bachelor's in Chemistry and Business from Westminster College, and specialized training in managed care pharmacy. His comprehensive understanding of the industry drives SmithRx's innovative approach to pharmacy benefits management.



